Role of Noroviruses in Sporadic Acute Gastroenteritis Cases from Children Attended in a Large Referral Childrenâ??s Hospital in Buenos Aires City, Argentina Buenos Aires City, Argentina
Angela Gentile*, Areso Maria Soledad, Juarez Maria del Valle, Orqueda Ana, Degiuseppe Juan Ignacio, Juan Andres, Turco, Marisa and Sabbaj Liliana
Published Date: 2022-06-28Angela Gentile1*, Areso Maria Soledad1, Juarez Maria del Valle1, Orqueda Ana1, Degiuseppe Juan Ignacio2, Juan Andres2, Turco, Marisa3 and Sabbaj Liliana4
1Department of Epidemiology, University of “Ricardo Gutiérrez”, Buenos Aires, Argentina
2Department of Rotavirus and Norovirus, National Institute of Infectious Diseases, Buenos Aires, Argentina
3Department of Bacteriology, University of “Ricardo Gutiérrez” Buenos Aires, Argentina
4Department of Norovirus, University of “Ricardo Gutiérrez” Buenos Aires, Argentina
- *Corresponding Author:
- Angela Gentile,
Department of Epidemiology,
University of “Ricardo Gutiérrez”, Buenos Aires,
Argentina,
Tel: 1130887431
E-mail:mrs.sedighehashemi@gmail.com
Received date: April 18, 2022, Manuscript No. IPPIDO-22-13201; Editor assigned date: April 21, 2022, PreQC No. IPPIDO-22-13201 (PQ); Reviewed date: May 06, 2022, QC No. IPPIDO-22-13201; Revised date: June 20, 2022, Manuscript No. IPPIDO-22-13201 (R); Published date: June 28, 2022, DOI: 10.36648/2573-0282.7.7.51
Citation: Gentile A, Soledad AM, Del Valle JM, Ana O, Juan D, et al. (2022) Role of Noroviruses in Sporadic Acute Gastroenteritis Cases from Children Attended in a Large Referral Children´s Hospital in Buenos Aires City, Argentina. Pediatric Infect Dis Vol:7 No:7
Abstract
Background: Noroviruses (NV) are recognized as the leading cause of sporadic and epidemic acute gastroenteritis worldwide, in all age groups. While there is increasing knowledge that NV is responsible for many acute gastroenteritis outbreaks in Argentina, studies to estimate prevalence in sporadic cases are scarce.
Methods: Descriptive, observational, cross-sectional study was conducted with children less than 5 years with acute gastroenteritis attending the outpatient department at the “Ricardo Gutiérrez” Children’s Hospital (RGCH) in Buenos Aires city between June 2017 and June 2021. Sociodemographic, clinical and epidemiological data were recorded. Stool samples were tested and genotyped for norovirus. Association between Norovirus detection and demographic and clinical variables was assessed.
Results: A total of 350 children with acute diarrhea were included, of which stool samples were collected for 332 (94.9%). Norovirus was detected in 81 cases (24.4%). Vomiting and moderate/severe diarrhea were more frequent in Norovirus positive than Norovirus negative children. However, presence of watery diarrhea and history of Rotavirus vaccination were significantly associated with Norovirus etiology. GII and GII.4 were the most frequently detected genogroup and genotype, respectively.
Conclusion: Noroviruses were detected with high frequency, mostly in children between 6 months and 2 years old, reinforcing the hypothesis of a new updated scenario of Norovirus predominance over Rotavirus. Watery diarrhea, complete vaccination against Rotavirus and vomiting are three key parameters that should raise suspicion of possible Norovirus gastroenteritis. Continuous and active Norovirus surveillance in this age group is important since children represent a priority group for Norovirus vaccine design and development.
Keywords
Diarrhea; Norovirus; Argentina; Children
Introduction
Acute diarrhea is still a major public health concern worldwide since it is associated with high morbidity and mortality in children under 5 years of age, particularly in developing countries [1]. Diarrheal diseases cause not only infections and death, but also malnutrition leading to stunting and cognitive impairment [2,3].
Etiological studies have shown the disease is caused mainly by viruses, especially in young children [4-7]. Rotaviruses and Noroviruses are widely described as the most common enteropathogens in children under 58. Moreover, in countries where universal Rotavirus vaccination has reached significant coverage levels, disease burden attributable to Norovirus (NV) is greater than that resulting from Rotavirus in the first years of life [8-13].
Noroviruses are recognized as the leading cause of sporadic and epidemic acute gastroenteritis worldwide, in all age groups, with high disease burden in young children, immunocompromised individuals, and the elderly [14]. This pathogen is responsible for over 200,000 deaths in children under 5 [15]. Recent studies in developing countries have described the presence of NV accounted for 15 to 30% of sporadic acute diarrheal episodes in both outpatient and hospital settings [16-18].
Noroviruses can be classified into genogroups based on complete VP1 amino acid sequences, of which GI and GII predominate in humans. Each genogroup can be further divided into genotypes based on nucleotide sequences of the capsid and polymerase regions [19]. GII.4 is the most frequently detected strain worldwide, associated with nearly 70% of the Norovirus infections. As GII.4 has shown epochal evolutionary dynamics, distinct variants are expected to emerge periodically replacing previous dominant strains [20].
In Argentina, around 1-1.25 million cases of acute gastroenteritis are reported each year in the public health sector, half of which occur in children under 5, resulting in a rate of 1,450 to 1,680 per 10,000 and Rotavirus has been identified as the most common etiological agent of diarrheal cases in that age group [21,22]. However, results from sentinel surveillance for gastroenteritis showed 40-60% of acute episodes in children remained undiagnosed [23]. After routine Rotavirus vaccination was incorporated to the national immunization program in 2015 (2 doses of monovalent vaccine at 2 and 4 months of age), rapid and significant decline in Rotavirus infection numbers was observed, suggesting NV could now be the leading cause of acute diarrhea in children, as has occurred in other countries after the introduction of Rotavirus vaccines [24].
While there is increasing knowledge that NV are responsible for many acute gastroenteritis outbreaks, few studies have been conducted to estimate prevalence in sporadic acute diarrhea cases in children, and the information on this in the last two decades is scarce [25-29].
The study aim was to assess the role of NV in sporadic acute diarrhea cases in children under 5 years of age attending the outpatient department at a large tertiary children´s hospital in Buenos Aires city, in order to contribute knowledge on the burden of Norovirus associated acute diarrhea and improve policies for disease control as well as accelerate vaccine development.
Materials and Methods
Study population
A descriptive, observational, cross-sectional study was conducted. Children under 5 years of age with symptomatic acute gastroenteritis attending the outpatient department at the “Ricardo Gutiérrez” Children’s Hospital (RGCH), one of the three largest pediatric referral centers in Buenos Aires city, between June 2017 and June 2021, were included.
Study enrollment was carried out through non-random convenience sampling to reduce potential selection bias. Data were recorded on case report forms detailing: demographics (age, gender), medical history and epidemiology (breastfeeding, premature birth, malnutrition or weight below 10th percentile, household members with diarrhea, daycare attendance), rotavirus vaccination (number of doses), diarrheal episode (date of symptom onset and of consultation, presence of vomiting, stool characteristics: watery/mucous/mucohemorrhagic/hemorrhagic, absent/mild/moderate/severe dehydration, prior antimicrobial treatment, and disease severity according to the vesikari score).
Stool samples were submitted to the argentine reference laboratory for viral gastroenteritis (INEI-ANLIS "Dr. Carlos G. Malbrán") for Norovirus testing and genotyping, as previously described. Briefly, after nucleic acid isolation (QIAampTM Viral RNA Mini Kit, Qiagen), samples were screened for NV GI and GII by a real-time quantitative reverse transcription polymerase chain reaction targeting the ORF1/ORF2 junction region (AgPath- IDTM One-Step RT-PCR, Applied Biosystems). Norovirus positive samples were further genotyped through amplification and sequencing of partial regions encompassing the 3’-end of the polymerase (RdRp) gene and the 5’-end of the capsid (VP1) genes (QiagenTM One-Step RT-PCR Kit, Qiagen). Genotype assignment of RdRp and VP1 partial sequences were obtained using the online software human calicivirus typing tool. Norovirus positive samples were additionally tested for other viral and bacterial enteropathogens using ELISA (Group A Rotavirus), RT-qPCR (sapovirus and astrovirus), qPCR (Group F adenovirus), and conventional culture with biochemical identification (Salmonella sp, Shigella sp, Campylobacter sp, diarrheagenic E. coli, Aeromonas sp, and Yersinia sp.) to determine presence of mixed infections.
Statistical analysis
For quantitative variables, calculation of median and Interquartile Range (IQR), or mean and standard deviation (and 95% confidence interval) was performed. Also, proportions for categorical variables were described. Wilcoxon rank sum or t-test (depending on the distribution of data), and Chi-square were used for continuous data and proportions, respectively.
Association between NV detection and demographic and clinical variables was assessed. The odds ratio and 95% Confidence Interval (95% CI) were used to measure potential association and p-value <0.05 considered statistically significant.
Results
From June 2017 to June 2021 a total of 350 children with acute diarrhea were identified and included in the study. Median age was 21.8 months (IQR:11-30 months) and 58.6% were males. Most of the children were eutrophic (98.3%) and 42.7% were breastfed. Seventy five (21.4%) children had at least one household member with diarrhea and 73.6% had been vaccinated for rotavirus (85.8% had received both doses). The most accompanying symptoms were fever (62.6%) and vomiting (54.3%). Fifty-six percent of patients presented watery diarrhea, followed by muco-hemorrhagic (42.6%), and hemorrhagic diarrhea (1.4%); 94.6% were well hydrated and no child suffered severe dehydration or shock. With respect to disease severity 41.4% were classified as mild, 49.4% as moderate, and as 9.2% severe according to the Vesikari Scoring System.
Oral rehydration solution and fluid therapy were prescribed in almost all patients (97.7%). Only eight patients were admitted for intravenous rehydration therapy.
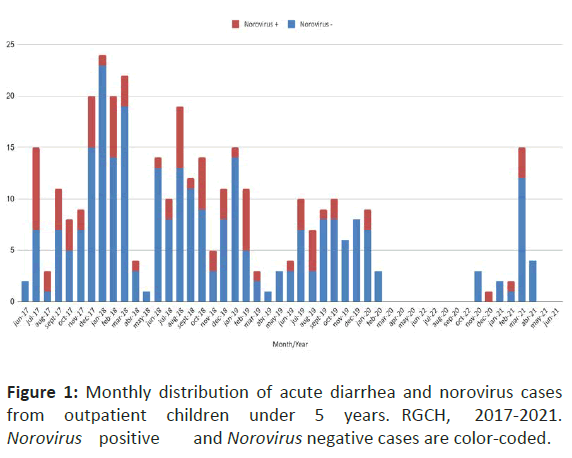
Even though acute diarrhea cases were uniformly distributed throughout the year, two seasonal were observed in consultations, January to March and June to August. In Argentina, the government implemented SARS-CoV-2 pandemic lockdown and distancing policies from March to November 2020, with ‘homeschooling’ as part of the adopted measures, producing a sharp decline in clinic visits related to diarrheal disease. Thus, as foreseeable, no outpatient came to hospital between March and October 2020 after the SARS-CoV-2 pandemic lockdown was implemented (Figure 1).
Stool samples were collected for 332 (94.9%) patients and NV was detected in 81 acute diarrhea cases (24.4%). Positive NV cases were evenly distributed throughout the year, although higher frequencies were observed in the months of July/August (2017-2019) and February (2018-2019). Sixty-five percent were male and the median age was 18.0 months (SD: 12.8 months); most cases (61.7%) occurred in children under 2 years, especially between 6 and 18 months of age (64.0%). With respect to epidemiological features, only 23.5% of positive cases referred a symptomatic household member, and 13.0% attended daycare; 84.8% had been vaccinated against Rotavirus, of which 90.7% had received two doses. Fever and vomiting were present in 55.6% and 61.7% of cases, respectively. Most Norovirus positive cases presented watery diarrhea (64.2%), followed by mucohemorrhagic (34.6%) and hemorrhagic (1.23%) stools. Although moderate/ severe diarrhea was present in 59.2%, almost all patients (95.1%) showed no significant loss of fluids and were sent home with information about monitoring for emergency signs, recommended home fluids or oral rehydration therapy.
Vomiting and moderate/severe diarrhea were more frequent in Norovirus positive than Norovirus negative children, but the difference was not statistically significant. Conversely, presence of watery diarrhea and history of Rotavirus vaccination were significantly associated with NV etiology (Table 1).
| Norovirus (+) (n=81) | Norovirus (-) (n=251) | OR (CI 95%) | P | |
|---|---|---|---|---|
| Sex (Male) | 65.40% | 55.80% | 1.5 (0.9-2.5) | 0.06 |
| Age (Months) (Median; IQR) | 18 | 19 | 0.59 | |
| (IQR= 11-27) | (IQR= 12-30) | |||
| Rotavirus vaccination (Yes) 2 doses | 84.80% | 69.60% | 2.4 (1.2-4.8) | 0.003 |
| 90.70% | 85.60% | 1.6 (0.6-4.6) | 0.17 | |
| Symptomatic household members (Yes) | 23.50% | 21.10% | 1.1 (0.6-2.1) | 0,33 |
| Fever (Yes) | 55.60% | 64.10% | 0.7 (0.4-1.2) | 0.08 |
| Vomiting (Yes) | 61.70% | 52.60% | 1,4 (0.9-2.4) | 0.07 |
| Watery diarrhea (Yes) | 64.20% | 46.20% | 1.5 (0.9-2.6) | 0.05 |
| Moderate and severe diarrhea (Vesikari scale) (Yes) | 59.30% | 41.00% | 1.0 (0.6-1.7) | 0.48 |
| Normally hydrated (Yes) | 95.10% | 94.00% | 1.2 (0.4-3.8) | 0.38 |
Table 1: Comparison of clinical and epidemiological characteristics between Norovirus positive and negative cases.
Of the samples that tested positive for NV, 27 (33.3%) showed bacterial coinfection. The most frequently isolated microorganisms were Campylobacter spp (13, 48.1%) followed by Shigella spp (9, 33.3%), Aeromonas spp (3, 11.1%), and diarrheagenic E. coli and Salmonella spp (1 case each, 3.7%). Yersinia spp coinfection was not detected among the Norovirus cases. Viral co-infections were detected in 5 cases with Rotavirus (6.2%), 5 with Astrovirus (6.2%), 4 with Group F Adenovirus (4.9%), and 3 with Sapovirus (3.7%). No Norovirus cases exhibited coinfection with two or more enteropathogens.
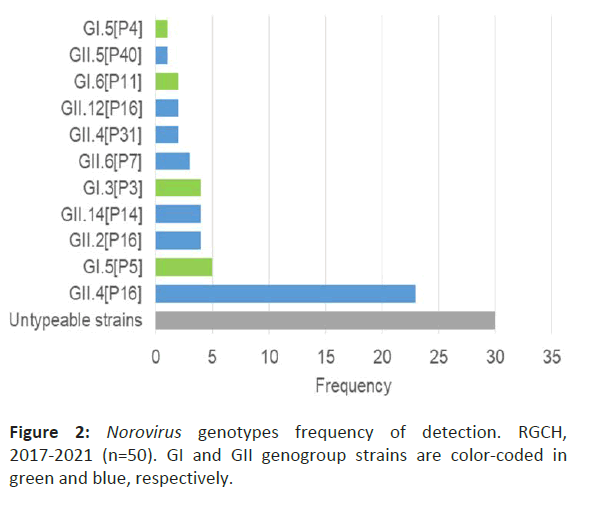
Genotyping showed 63 NV (77.8%) were GII, 17 (21.0%) GI, and 1 (1.2%) was a mixed GI/GII infection. Six different genotypes were identified for GII (GII.2, GII.4, GII.5, GII.6, GII.12, and GII.14) and 3 for GI (GI.3, GI.5, and GI.6). The most frequent genotypes were GII.4 Sydney [P16] (28.4%), GII.2 [P16] (4.9%), and GII.14 [P7] (4.9%) for GII strains, and GI.5 [P5] (6.2%) and GI.3 [P3] (4.9%) for GI strains. Of note, in 29 (35.8%) strains the genotype could not be identified (Figure 2).
Discussion
In this study we assessed the role of norovirus as the cause of acute symptomatic gastroenteritis in children less than 5 years of age, treated as outpatients at a large tertiary referral children´s hospital in Buenos Aires city. Overall, NV was detected in 24.4% of stool samples analyzed. These results are in agreement with those of recent studies conducted in Argentina and Latin America through both active and passive surveillance programs [30]. We detected NV cases throughout the year, with higher rates during warmer and colder months. This seasonal pattern differs from other studies describing a single winter peak [31]. Highest prevalence occurred in children between 6 months and 2 years old, the same age group classically affected by Rotavirus, reinforcing the hypothesis of a new updated scenario of Norovirus predominance over Rotavirus, especially in countries with optimal Rotavirus vaccination coverage [32].
Our results describe the clinical and epidemiological profile of NV infections in a sample population of children under 5 years of age. However, they only represent a very small fraction of the total number of cases, as acute diarrhea is generally underreported [33]. With respect to NV in particular, lack of accessible diagnostic methods at most healthcare centers further undermines estimates on the role of this pathogen as a common etiological agent. In this study, patients who developed watery diarrhea and had complete vaccination against Rotavirus were likely to have Norovirus infection. Although not statiscally significant, many of the cases also presented vomiting. These three parameters, when present, should raise suspicion of possible NV gastroenteritis.
Also noteworthy, was the high proportion of both bacterial and viral coinfections among Norovirus cases. While coinfections have been extensively described in developing countries, the contribution of multiple enteropathogens to disease severity and prognosis remains under debate [34-36]. In our study, Norovirus cases with bacterial and viral coinfections were more associated with moderate and severe than to mild cases (P-value= 0.028).
Analysis of viral diversity showed GII was the most predominant geno group and GII.4 was found in one third of the positive cases. As in previous studies, genotypes found in sporadic cases were more diverse than those associated with outbreaks [37,38]. Moreover, polymerase genotype GII.P16 was detected in association with GII.2, GII.4 and GII.12 capsid genotypes. Spread of this polymerase occurred rapidly after its association with GII.4 Sydney during the 2015-2016 seasons. It is thought to have significant epidemic potential due to its ability to generate recombinant strains with several genotypes [39]. Twenty nine Norovirus strains could not be genotyped as it was not possible to amplify or sequence the specific target for dual genotyping, mainly because viral loads in stool samples were low, and correlated with higher RT-qPCR Ct values (>30) compared to genotyped strains (data not shown). Interactions between viral load and host-related factors, pathogens, transmission mode and timing of specimen collection remain unclear. Since our population comprised immunocompetent, ambulatory patients, predominance of mild episodes could help explain the high Ct values.
Conclusion
Continuous and active NV surveillance in children is important for several reasons. First, as Rotavirus vaccines have been increasingly incorporated into National Immunization Programs, Norovirus is becoming more prevalent as the leading cause of acute gastroenteritis. Second, it has been proposed that children are reservoirs of genetic diversity; therefore early detection could allow identification of emerging strains with pandemic potential circulating before detection during outbreaks. Also, as with other high-risk populations, children represent a priority group for norovirus vaccine design and development, to prevent and control the increasing burden of disease.
During the course of the COVID-19 pandemic in 2020, acute gastroenteritis episodes declined. It was assumed that Norovirus cases had decreased as well. Conversely, in the first semester of 2021, Norovirus infections increased, probably because social activities and schools reopened, as restrictions implemented during the COVID-19 lockdown were loosened. For this reason, active monitoring of acute diarrhea and Norovirus infections is important in the post pandemic scenario, during which improved personal hygiene measures such as hand washing were put into practice, but rates of routine rotavirus vaccination fell.
Acknowledgements
We would like to thank Karina Rivero for her technical assistance at Argentina Reference Laboratory for Rotavirus and Norovirus, and Cynthia Vartalitis from ‘Ricardo Gutierrez’ Children´s Hospital for her critical review and English editing of the manuscript.
Funding
This work was supported by Takeda Vaccines Inc. The sponsor provided some input on the study design and operations of this study. The authors had responsibility for the submission of this manuscript for publication.
Conflict of interest
The authors have no conflicts of interest to disclose.
References
- Troeger CE, Khalil IA, Blacker BF, Biehl MH, Albertson SB, et al. (2020) Quantifying risks and interventions that have affected the burden of diarrhoea among children younger than 5 years: an analysis of the Global Burden of Disease Study 2017. Lancet Infect Dis 20:37–59
[Crossref] [Googlescholar] [Indexed]
- Briend A, Collins S (2010) Therapeutic nutrition for children with severe acute malnutrition summary of African experience. Indian Pediatr 47:655–659
[Crossref] [Googlescholar] [Indexed]
- Nahar B, Ahmed T, Brown KH, Hossain MI (2010) Risk factors associated with severe underweight among young children reporting to a diarrhoea treatment facility in Bangladesh. J Health Popul Nutr 28:476–483
[Crossref] [Googlescholar] [Indexed]
- Poulain C, Galeno H, Loayza S, Vergara N, Valdivieso F, et al. (2021) Molecular detection of gastrointestinal pathogens among children under 5 years old with diarrhea in a hospital center for rotavirus sentinel surveillance in Chile. Rev Chilena Infectol 38:54–60
[Crossref] [Googlescholar] [Indexed]
- Trivedi TK, de Salvo T, Lee L, Palumbo A, Moll M, et al. (2012) Hospitalizations and mortality associated with norovirus outbreaks in nursing homes, 2009-2010. JAMA 308:1668–1675
[Crossref] [Googlescholar] [Indexed]
- Patel MM, Hall AJ, Vinje J, Parashar UD (2009) Noroviruses: a comprehensive review. J Clin Virol 44:1–8
[Crossref] [Googlescholar] [Indexed]
- Platts-Mills JA, Babji S, Bodhidatta L (2015) Pathogen-specific burdens of community diarrhoea in developing countries: a multisite birth cohort study (MAL-ED). Lancet Glob Health 3:564-575
[Crossref] [Googlescholar] [Indexed]
- Lopman BA, Steele D, Kirkwood CD, Parashar UD (2016) The Vast and Varied Global Burden of Norovirus: Prospects for Prevention and Control. PLoS Med 13:1001999
[Crossref] [Googlescholar] [Indexed]
- Payne DC, Vinje J, Szilagyi PG, et al. (2013) Norovirus and medically attended gastroenteritis in U.S. children. N Engl J Med 368:1121–1130
[Crossref] [Googlescholar] [Indexed]
- Santos VS, Berezin EN, Gurgel RQ (2017) Rotavirus in Latin America: Current Situation and Perspectives. J Pediatr Infect Dis Soc 6:1–2
[Crossref] [Googlescholar] [Indexed]
- Becker-Dreps S, Bucardo F, Vilchez S, Zambrana LE, Liu L, et al. (2014) Etiology of childhood diarrhea after rotavirus vaccine introduction: a prospective, population-based study in Nicaragua. Pediatr Infect Dis J 33:1156–1163
[Crossref] [Googlescholar] [Indexed]
- Hemming M, Rasanen S, Huhti L, Paloniemi M, Salminen M, et al. (2013) Major reduction of rotavirus, but not norovirus, gastroenteritis in children seen in hospital after the introduction of RotaTeq vaccine into the National Immunization Programme in Finland. Eur J Pediatr 172:739–746
[Crossref] [Googlescholar] [Indexed]
- McAtee CL, Webman R, Gilman RH, Mejia C, Bern C, et al. (2016) Burden of Norovirus and Rotavirus in Children after Rotavirus Vaccine Introduction, Cochabamba, Bolivia. Am J Trop Med Hyg 94:212–217
[Crossref] [Googlescholar] [Indexed]
- Ahmed SM, Hall AJ, Robinson AE, Verhoef L, Premkumar P, et al. (2014) Global prevalence of norovirus in cases of gastroenteritis: a systematic review and meta-analysis. Lancet Infect Dis 14:725–730
[Crossref] [Googlescholar] [Indexed]
- Patel MM, Widdowson MA, Glass RI, Akazawa K, Vinje J, et al. (2008) Systematic literature review of role of noroviruses in sporadic gastroenteritis. Emerg Infect Dis 14:1224–1231
[Crossref] [Googlescholar] [Indexed]
- O’Ryan M, Riera-Montes M, Lopman B (2017) Norovirus in Latin America: Systematic Review and Meta-analysis. Pediatr Infect Dis J 36:127–134
[Crossref] [Googlescholar] [Indexed]
- Sarmento SK, de Andrade J da SR, Miagostovich MP, Fumian TM (2021) Virological and Epidemiological Features of Norovirus Infections in Brazil, 2017-2018. Viruses 13:1724
[Crossref] [Googlescholar] [Indexed]
- Safadi MA, Riera-Montes M, Bravo L, Tangsathapornpong A, Lagos R, et al. (2021) The burden of norovirus disease in children: a multi-country study in Chile, Brazil, Thailand and the Philippines. Int J Infect Dis 109:77–84
[Crossref] [Googlescholar] [Indexed]
- Chhabra P, de Graaf M, Parra GI, Chan MC, Green K, et al. (2019) Updated classification of norovirus genogroups and genotypes. J Gen Virol 100:1393–1406
[Crossref] [Googlescholar] [Indexed]
- Zakikhany K, Allen DJ, Brown D, Iturriza-Gomara M (2012) Molecular evolution of GII-4 Norovirus strains. PloS One 7:41625
[Crossref] [Googlescholar] [Indexed]
- Degiuseppe JI, Giovacchini C, Stupka JA (2013) Rotavirus epidemiology and surveillance in Argentina: 2009-2011. Arch Argent Pediatr 111:148–154
[Crossref] [Googlescholar] [Indexed]
- Degiuseppe JI, Reale EA, Stupka JA (2017) Rotavirus epidemiology and surveillance before vaccine introduction in Argentina, 2012-2014. J Med Virol 89:423–428
[Crossref] [Googlescholar] [Indexed]
- Degiuseppe JI, Stupka JA (2018) First assessment of all-cause acute diarrhoea and rotavirus-confirmed cases following massive vaccination in Argentina. Epidemiol Infect 146:1948–1954
[Crossref] [Googlescholar] [Indexed]
- Degiuseppe JI, Barclay L, Gomes KA, Costantini V, Vinje J, et al. (2020) Molecular epidemiology of norovirus outbreaks in Argentina, 2013-2018. J Med Virol 92:1330–1333
[Crossref] [Googlescholar] [Indexed]
- Gomes KA, Stupka JA, Gomez J, Parra GI (2007) Molecular characterization of calicivirus strains detected in outbreaks of gastroenteritis in Argentina. J Med Virol 79:1703–1709
[Crossref] [Googlescholar] [Indexed]
- Gomes KA, Stupka JA, Diana A, Parra GI (2008) Molecular characterization of calicivirus strains detected in outbreaks of gastroenteritis occurring in Argentina during 2005 and 2006]. Rev Argent Microbiol 40:222–228
[Googlescholar] [Indexed]
- Bereciartu A, Bok K, Gomez J (2002) Identification of viral agents causing gastroenteritis among children in Buenos Aires, Argentina. J Clin Virol 25:197–203
[Crossref] [Googlescholar] [Indexed]
- Martinez N, Espul C, Cuello H, Zhong W, Jiang X, et al. (2002) Sequence diversity of human caliciviruses recovered from children with diarrhea in Mendoza, Argentina, 1995-1998. J Med Virol 67:289–298
[Crossref] [Googlescholar] [Indexed]
- Degiuseppe JI, Roitman KL, Rivero KA, Stupka JA (2021) Norovirus passive surveillance as an alternative strategy for genetic diversity assessment in developing countries. J Infect Public Health 14:990–993
[Crossref] [Googlescholar] [Indexed]
- Hall AJ, Vinje J, Lopman B, Park GW, Yen C, et al. (2011) Updated norovirus outbreak management and disease prevention guidelines. Morb Mortal Wkly Rep 60:1–18
[Googlescholar] [Indexed]
- Santos VS, Gurgel RQ, Cavalcante SMM, Kirby A, Cafe LP, et al. (2017) Acute norovirus gastroenteritis in children in a highly rotavirus-vaccinated population in Northeast Brazil. J Clin Virol 88:33–38
[Crossref] [Googlescholar] [Indexed]
- Scallan E, Jones TF, Cronquist A, Thomas S, Frenzen P, et al. (2006) Factors associated with seeking medical care and submitting a stool sample in estimating the burden of foodborne illness. Foodborne Pathog Dis 3:432–438
[Crossref] [Googlescholar] [Indexed]
- Kotloff KL (2017) The Burden and Etiology of Diarrheal Illness in Developing Countries. Pediatr Clin North Am 64:799–814
[Crossref] [Googlescholar] [Indexed]
- Paniagua GL, Monroy E, Garcia-Gonzalez O, Alonso J, Negrete E, et al. (2007) Two or more enteropathogens are associated with diarrhoea in Mexican children. Ann Clin Microbiol Antimicrob 6:17
[Crossref] [Googlescholar] [Indexed]
- Farfan-Garcia AE, Imdad A, Zhang C, Arias-Guerrero MY, Sanchez-Alvarez NT, et al. (2020) Etiology of acute gastroenteritis among children less than 5 years of age in Bucaramanga, Colombia: A case-control study. PLoS Negl Trop Dis 14:0008375
[Crossref] [Googlescholar] [Indexed]
- Allen DJ, Trainor E, Callaghan A, O'Brien SJ, Cunliffe NA, et al. (2016) Early Detection of Epidemic GII-4 Norovirus Strains in UK and Malawi: Role of Surveillance of Sporadic Acute Gastroenteritis in Anticipating Global Epidemics. PloS One 11:0146972
[Crossref] [Googlescholar] [Indexed]
- Kremer JR, Langlet J, Skraber S, Weicherding P, Cauchie HM, et al. (2011) Genetic diversity of noroviruses from outbreaks, sporadic cases and wastewater in Luxembourg 2008-2009. Clin Microbiol Infect 17:1173–1176
[Crossref] [Googlescholar] [Indexed]
- Barclay L, Cannon JL, Wikswo ME, Phillips AR, Browne H, et al. (2019) Emerging Novel GII.P16 Noroviruses Associated with Multiple Capsid Genotypes. Viruses 11:535
[Crossref] [Googlescholar] [Indexed]
- Shioda K, Barclay L, Becker-Dreps S, Bucardo-Rivera F, Cooper PJ, et al. (2017) Can Use of Viral Load Improve Norovirus Clinical Diagnosis and Disease Attribution? Open Forum Infect Dis 4:ofx131
[Crossref] [Googlescholar] [Indexed]
Open Access Journals
- Aquaculture & Veterinary Science
- Chemistry & Chemical Sciences
- Clinical Sciences
- Engineering
- General Science
- Genetics & Molecular Biology
- Health Care & Nursing
- Immunology & Microbiology
- Materials Science
- Mathematics & Physics
- Medical Sciences
- Neurology & Psychiatry
- Oncology & Cancer Science
- Pharmaceutical Sciences